When Home Is No Longer Enough: Signs It’s Time for Long-Term Care
Originally published: May 2026 | Reviewed by Sadie Mays
Originally published: May 2026 | Reviewed by Sadie Mays

Recognizing that a parent or spouse needs more help than you can provide at home is one of the most emotionally difficult realizations a family faces. Most families arrive at this decision after a crisis — a fall, a hospitalization, a close call with the stove — when proactive observation could have made the transition safer and less disorienting for everyone involved.
A single fall becomes “she just tripped.” A missed medication becomes “he’s been forgetting things for years.” Individual signs form a pattern that clearly points to a level of care that home management can no longer safely provide — and proactive observation means watching for that pattern over weeks and months, rather than reacting to incidents after the fact.
Reactive decision-making — choosing a skilled nursing facility during the 48 hours after a hospitalization — produces worse placement outcomes than decisions made with time, research, and family alignment.
Falls are the leading cause of injury-related death among adults 65 and older, according to the Centers for Disease Control and Prevention, and the home environment is where the majority of those falls occur. Safety concerns that repeat without resolution are among the clearest indicators that professional long-term care has become necessary.
Difficulty transferring — getting in and out of bed, rising from a chair, or stepping in and out of a shower — is one of the most reliable early indicators of fall risk in aging adults.
A person who can no longer complete these movements independently or with minimal assistance faces daily injury exposure that a family caregiver without clinical training cannot safely manage.
Watch whether your loved one avoids certain movements, grips furniture for balance during routine tasks, or spends significantly more time in bed than they did six months ago. Each of these behaviors indicates that the gap between mobility capacity and home environment has widened past the point of safe management.
Frequent bruising, skin tears, or minor falls that a loved one minimizes or conceals are clinical warning signs, not incidental events. Older adults with balance disorders, peripheral neuropathy, or early cognitive decline often underreport falls because they fear losing independence.
A family member who notices new bruising on the arms, legs, or hips — particularly on the side of the body consistent with a lateral fall — should treat that observation as meaningful data.
The fall-prevention research consistently shows that a first fall significantly increases the likelihood of a second; a pattern of concealed falls indicates a home environment that has already become unsafe.
Many traditional homes in Atlanta’s established neighborhoods — Cascade Heights, Collier Hills, Druid Hills — were built with bedrooms on upper floors and laundry in basements.
An aging adult with reduced mobility, reduced cardiovascular reserve, or early cognitive decline faces compounding risks in these environments: stair-related falls, isolation on a single floor, and inability to access outdoor space independently.
When a loved one begins sleeping in a recliner rather than climbing stairs to a bedroom, or avoids the kitchen because it requires navigating a difficult space, the home’s physical structure has become a clinical liability.
If you’re ready to get started, call us now!

Medication mismanagement is among the most reliably observable early warning signs of cognitive or functional decline — and among the most dangerous, because the consequences of dosing errors compound silently before they become visible.
Forgetting to take a daily medication and accidentally taking a double dose represent opposite ends of the same failure: a person can no longer reliably track a medication schedule without external structure.
For older adults managing hypertension, heart failure, or anticoagulation therapy, both errors carry serious clinical consequences. A missed dose of a blood thinner on Monday and a double dose on Tuesday do not average out — each error is an independent risk event.
Ask your loved one’s pharmacist whether refill patterns are consistent with the prescribed dosing schedule; irregular refill timing often surfaces dosing problems before a family member notices them at home.
New prescriptions that require strict timing — insulin administered before meals, heart failure medications taken at specific intervals, inhalers used in a defined sequence — place demands on working memory and executive function that cognitive decline directly impairs.
Older adults managing multiple daily medications with varying schedules face an organizational burden that exceeds what many cognitively intact adults handle reliably without a system. When that organizational demand meets early memory loss, the risk of a serious adverse event rises substantially. Facilities providing long-term care use licensed nurses and electronic medication administration records to eliminate this category of risk entirely.
Finding multiple expired medication bottles in a medicine cabinet, or discovering that a prescription written months ago was never filled, indicates that a loved one has stopped managing their own medication regimen — whether because of cognitive decline, mobility barriers to reaching a pharmacy, or a decision to discontinue treatment without telling anyone.
Unfilled prescriptions for chronic conditions like COPD or diabetes are not administrative oversights; they are interruptions in disease management that produce clinical deterioration.
A systematic check of a loved one’s medicine cabinet during a home visit often reveals this pattern before any other sign becomes visible.
Chronic illness management and functional decline follow predictable trajectories that families can learn to read. These three patterns carry the most clinical significance when evaluating whether home care remains appropriate.
Congestive heart failure, chronic obstructive pulmonary disease, and insulin-dependent diabetes each require daily monitoring — weight checks, oxygen saturation readings, blood glucose logs — that a family caregiver without clinical training cannot reliably interpret or act on.
A CHF patient who gains three pounds in 48 hours needs a clinical response, not reassurance. A COPD patient whose baseline oxygen saturation has dropped two points over a week needs a physician assessment, not a wait-and-see approach.
When a chronic condition has reached the stage where daily monitoring requires clinical interpretation, the level of care has exceeded what home management can safely provide. Sadie G. Mays Health & Rehabilitation Center’s nursing services are structured specifically for this level of medically complex long-term care.
A pattern of recurring hospitalizations — discharge, brief home recovery, decline, rehospitalization — indicates that the home environment is not providing sufficient support to maintain the baseline health status achieved during each hospital stay.
The 30-day hospital readmission rate for Medicare beneficiaries with heart failure, pneumonia, and COPD is a federally tracked quality measure under the Hospital Readmissions Reduction Program precisely because readmission signals inadequate post-discharge support.
Families who recognize this revolving-door pattern are observing a care gap that post-hospital rehab in a skilled nursing setting is specifically designed to close.
Activities of daily living — bathing, dressing, toileting, transferring, and eating — are the functional baseline measures used by physicians and care managers to assess independence.
When a loved one begins skipping showers, wearing the same clothing for multiple days, or showing visible signs of poor hygiene without explanation, ADL decline becomes apparent from the outside.
The transition point from home care to skilled nursing versus assisted living is typically reached when two or more ADLs require daily hands-on physical assistance.
If you’re ready to get started, call us now!
Cognitive decline poses safety risks qualitatively different from physical decline — they are less visible, more variable day-to-day, and more likely to lead to a serious incident without warning.
A loved one who has become disoriented in familiar Atlanta neighborhoods — walking to a store visited for decades and being unable to find the way back — has reached a stage of cognitive decline that home supervision alone cannot safely manage. Wandering is not limited to nighttime or to people with advanced dementia; it occurs across the middle stages of Alzheimer’s disease and related dementias, often during transitions between activities or at times when the person is fatigued.
The Alzheimer’s Association estimates that six in ten people with dementia will wander at some point during the course of the disease. Dedicated memory care settings use secured environments, wander-guard technology, and structured daily programming to eliminate this risk.
Increased agitation in the late afternoon and evening — clinically described as sundowning — paranoia toward family members, or accusations of theft are behavioral symptoms of cognitive decline that exceed what most family caregivers can safely and sustainably manage at home.
These behaviors are not willful and are not directed at the caregiver personally, but they produce significant caregiver distress and carry physical safety risks for both the person with dementia and the people caring for them.
Understanding the stages of Alzheimer’s disease helps families recognize where behavioral changes fit in the progression and what level of care that stage typically requires.
Unpaid utility bills discovered by chance, a pattern of writing checks for incorrect amounts, or a loved one who has become a repeated target of phone scams are financial behaviors that signal executive function impairment — the cognitive capacity to plan, sequence, and monitor multi-step tasks.
Executive function decline typically precedes more visible memory symptoms, meaning financial lapses often appear before a family recognizes cognitive decline.
A loved one who has lost track of bank balances, failed to reconcile statements, or made large, unexplained cash withdrawals requires both a medical evaluation and an immediate review of financial safeguards.
Caregiver burnout is a medical condition with clinical consequences for the caregiver, not a measure of insufficient love or commitment. Recognizing it early protects both the caregiver and the person receiving care.
Family caregivers who develop back injuries from repeated transfers, who sleep fewer than six hours per night due to nighttime caregiving demands, or who have discontinued their own medical appointments because caregiving leaves no time are experiencing physical deterioration that will eventually impair their ability to provide care entirely.
Research from the National Alliance for Caregiving consistently documents higher rates of poor self-reported health among family caregivers than among non-caregivers. A caregiver whose physical health is declining cannot sustainably provide the level of care a medically complex older adult requires.
Persistent feelings of resentment toward the person receiving care, chronic anxiety about what might happen when the caregiver is not present, and progressive withdrawal from friendships and personal activities are the emotional signature of advanced caregiver burnout.
These feelings are predictable physiological and psychological responses to a sustained high-demand caregiving role without adequate support or respite — not evidence of a character failing.
Families who recognize these signs should treat them with the same clinical seriousness they would apply to a loved one’s physical symptoms. Respite care provides structured, short-term relief that interrupts the progression of burnout before it reaches a breaking point.
When a family caregiver regularly misses work to respond to caregiving emergencies, declines professional responsibilities, or makes decisions that jeopardize their employment stability, the caregiving arrangement has expanded beyond a sustainable boundary.
The financial consequences of reduced income or job loss — compounded by the direct costs of home caregiving — often exceed the cost of professional long-term care when calculated honestly over a 12-month horizon.
A caregiver managing their own children, marriage, and career alongside full-time caregiving is carrying a combination of demands that no single person can sustain indefinitely without structural support.
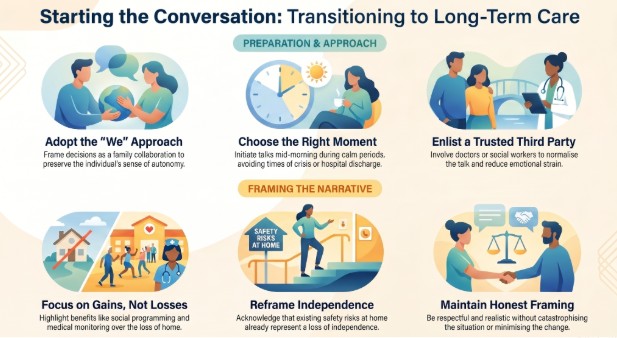
The conversation about transitioning to long-term care is most productive when it happens before a crisis makes it unavoidable. Timing, framing, and language all shape whether the conversation produces alignment or resistance.
Framing the conversation around shared family decision-making — “we want to make sure you’re safe” rather than “you need to move” — reduces the likelihood that a parent hears the discussion as an ultimatum or a loss of autonomy.
The “we” approach positions the transition as something the family is navigating together rather than something being done to the person who needs care. Families who have reviewed how to talk to a parent about moving into long-term care consistently report that language choices make a significant difference in whether the initial conversation opens or closes a dialogue.
The right moment for this conversation is a calm, private setting when neither party is in crisis, fatigued, or recently discharged from a hospital. A conversation initiated in an emergency room or immediately after a fall produces fear-driven decisions rather than considered ones.
Choose a time when your loved one is at their cognitive best — typically mid-morning for most older adults — and frame the discussion as a conversation, not an announcement. Bringing a trusted third party — a family physician, a geriatric care manager, or a social worker — normalizes the conversation and distributes the emotional weight away from the family relationship.
Reframing the transition around what a loved one gains — consistent medical monitoring, social programming, freedom from home maintenance, and access to rehabilitative services — addresses the core fear driving most resistance: that moving to a care facility means losing independence and identity.
A person who currently cannot safely shower without assistance has already lost a degree of independence; the question is whether that loss is managed safely by clinical professionals or unsafely at home.
Honest framing that acknowledges this reality — respectfully and without catastrophizing — produces more productive conversations than reassurances that minimize the scope of the transition.
Families who recognize these signs early and act on them give their loved ones something that reactive crisis decisions cannot: time to participate in the choice, time to visit facilities, and time to adjust to a transition made thoughtfully rather than under duress.
Consulting a primary care physician for a formal functional assessment — or working with a geriatric care manager who can evaluate ADL capacity, cognitive status, and home safety simultaneously — removes the burden of clinical judgment from family members who are not equipped to make it alone.
Sadie G. Mays Health & Rehabilitation Center serves families across Atlanta who are navigating exactly this transition.
Contact our admissions team to discuss care options, schedule a tour, or ask questions about what the right level of care looks like for your loved one’s specific situation.
What are the most common signs that a parent needs long-term care?
The most common signs that a parent needs long-term care include repeated falls, medication management errors, worsening chronic illness, ADL decline in bathing or dressing, cognitive changes such as wandering or sundowning, and visible caregiver burnout in the family members providing care at home.
How do falls indicate that long-term care is needed?
Falls indicate a need for long-term care when they occur repeatedly, when injuries are minimized or concealed, or when the home environment cannot be modified to address the underlying mobility or balance impairment. A second fall following a first significantly increases the statistical risk of a serious injury.
What is ADL decline, and why does it matter for long-term care decisions?
ADL decline refers to a deterioration in the ability to independently perform activities of daily living — bathing, dressing, toileting, transferring, and eating. When two or more ADLs require daily hands-on physical assistance, the care level has typically exceeded what a family caregiver can safely provide without clinical training.
What is caregiver burnout, and how does it affect the decision to seek long-term care?
Caregiver burnout is a state of physical, emotional, and social exhaustion produced by sustained high-demand caregiving without adequate support. Burnout affects care quality and creates independent health risks for the caregiver, making it a legitimate clinical reason to transition to professional long-term care.
When should a family talk to a doctor about long-term care for a parent?
A family should talk to a physician about long-term care when a parent shows repeated falls, medication errors, unexplained cognitive or behavioral changes, frequent hospitalizations, or ADL decline. A primary care physician or geriatric care manager can provide a formal functional assessment that guides the placement decision.
What is sundowning, and why is it a sign that long-term care is needed?
Sundowning is a pattern of increased agitation, confusion, and behavioral disturbance in people with dementia that intensifies in the late afternoon and evening hours. Sundowning creates safety risks that home supervision alone typically cannot manage and is a clinical indicator that dedicated memory care has become appropriate.
How do you talk to a parent about moving to a long-term care facility?
Talk to a parent about moving to a long-term care facility using “we” language that frames the decision as a shared family choice, choose a calm mid-morning moment when the person is at their cognitive best, and focus the conversation on safety gains and access to care rather than on what is being left behind.
What is a geriatric care manager, and how can one help with the long-term care decision?
A geriatric care manager is a licensed health professional — typically a nurse or social worker — who specializes in assessing the functional, cognitive, and social needs of aging adults. A geriatric care manager conducts a formal evaluation of home safety, ADL capacity, and medical complexity, then recommends an appropriate level of care.